Sign up for the latest updates from Luvo.
Thank you for joining us! We'll keep you posted with more updates.
By clicking “Subscribe” you agree to our Terms and Conditions and Privacy Policy.
weight loss
Microdosing
Testosterone
Hormone Replacement




Testosterone isn’t just a “men’s hormone.” Women make it too, and levels can decline with age, surgical menopause, or hormonal shifts. For some postmenopausal women, that drop is linked to persistent low sexual desire with distress (often called HSDD), even after addressing common contributors like vaginal dryness, sleep, stress, mood, medications, and relationship factors.
Get startedTestosterone – systemic androgen therapy designed to deliver steady, low-dose testosterone through the skin. Clinical best practice is to maintain female physiologic blood levels, not “high” or “performance” dosing.
Because testosterone products are often formulated for men, women’s therapy requires individualized dosing and careful titration. If prescribed, your clinician will:
Side effects are more likely if testosterone levels rise above the physiologic female range. Possible effects include:
Testosterone Gel is a prescription hormone therapy used in menopause care primarily for postmenopausal women diagnosed with HSDD (low sexual desire that causes personal distress) after a biopsychosocial assessment. Current consensus statements emphasize that this is the only evidence-based indication for testosterone therapy in women.

Images are for illustrative purposes only. Individual results may vary. Compounded medications are not FDA-approved.
Desire is multi-factorial—hormones are only one piece. When testosterone is truly low and other contributors are addressed, restoring testosterone to the physiologic female range may help support the neurobiological pathways involved in sexual interest and responsiveness. In clinical studies of transdermal testosterone for HSDD, women experienced improvements in desire and reduced distress compared with placebo.

Images are for illustrative purposes only. Individual results may vary. Compounded medications are not FDA-approved.
Testosterone gel is applied to clean, dry skin and allowed to fully dry. Because topical testosterone can transfer via skin contact, safety steps matter: wash hands after applying, cover the application site with clothing once dry, and wash the site before skin-to-skin contact.
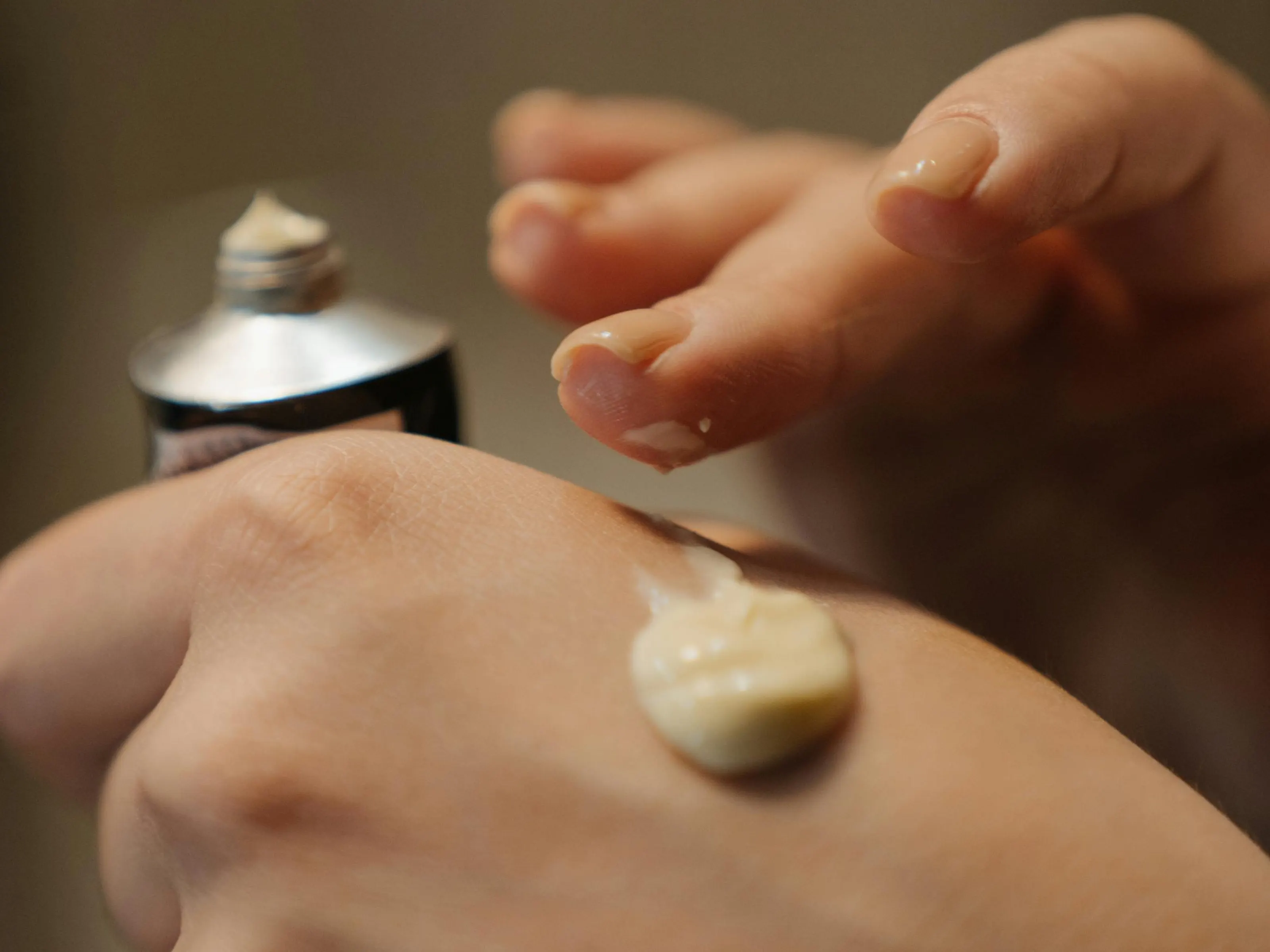
Images are for illustrative purposes only. Individual results may vary. Compounded medications are not FDA-approved.


Testosterone gel is a prescription, topical form of testosterone applied to the skin. For some women in peri-/menopause, it may be used to support symptoms linked to low androgen levels, most commonly low libido, low energy, and reduced sense of well-being.
Many women prefer gel because it’s non-invasive and easy to use at home. It can also offer steadier day-to-day dosing. The best option depends on your symptoms, lab values, and what fits your routine.
Testosterone therapy is most often considered for low sexual desire, reduced arousal, low energy, decreased motivation, and difficulty maintaining strength. Results vary, and treatment should be guided by both symptoms and lab monitoring.
Some women notice subtle changes in energy or mood within a few weeks. Libido and performance-related changes often take longer. Many clinicians reassess around 6–12 weeks to evaluate response and adjust dosing if needed.
You’ll apply it exactly as prescribed (usually once daily) onto clean, dry skin. The most important part is consistency: apply at the same time each day and follow your clinician’s instructions on placement and amount.
Yes, skin-to-skin transfer is possible until the gel fully dries and the area is covered. Let it dry completely, wash your hands after applying, and follow guidance on clothing coverage and timing before close contact.
Yes. Baseline labs help confirm whether testosterone is appropriate and guide safe dosing. Follow-up labs help ensure your levels stay in a healthy range for women and reduce the risk of side effects.
Not necessarily. In appropriate doses, testosterone may support strength and body composition for some women. However, hormones can influence appetite, water retention, sleep, and energy, so your plan should include monitoring and lifestyle support.
Side effects are often dose-related and may include acne, oily skin, increased facial/body hair, scalp hair thinning (in those predisposed), and mood or sleep changes. If side effects appear, your clinician can adjust your dose.
These effects are uncommon at carefully managed, female-appropriate dosing, but they can occur if levels run too high. Report early signs (voice changes, increased hair growth, clitoral sensitivity changes) promptly so your clinician can reassess.
Often, yes. Many menopause plans include estrogen and progesterone, and testosterone may be added when appropriate. Your clinician will tailor the combination based on symptoms, labs, and medical history.
Testosterone may not be appropriate if you’re pregnant or breastfeeding, have certain hormone-sensitive conditions, or have uncontrolled medical issues that require stabilization first. Your clinician will review your history and help choose the safest option.м