Sign up for the latest updates from Luvo.
Thank you for joining us! We'll keep you posted with more updates.
By clicking “Subscribe” you agree to our Terms and Conditions and Privacy Policy.
Microdosing
Testosterone
Hormone Replacement



Ozempic® Injection is a once-weekly prescription medication designed to support blood sugar regulation and metabolic health. Under clinician guidance, it may also support sustainable weight management as part of a comprehensive care plan that includes nutrition and lifestyle adjustments.
Get startedOzempic® contains semaglutide, a prescription GLP-1 receptor agonist. Semaglutide works by activating GLP-1 receptors to help improve blood sugar control in adults with type 2 diabetes. It supports glucose regulation by increasing insulin release when blood sugar is high, reducing glucagon when appropriate, and slowing gastric emptying, which can reduce post-meal blood sugar spikes. Some people may also experience appetite-related effects while taking Ozempic®.
Ozempic® is taken once weekly, on the same day each week, at any time of day, with or without food. It is injected subcutaneously (under the skin) using the Ozempic® pen.
Where to inject: abdomen (stomach area), thigh, or upper arm. Rotate injection sites each week and avoid injecting into areas that are tender, bruised, red, or hard.
If you miss a dose, follow the instructions in the Ozempic® Medication Guide and your clinician’s guidance. Do not take extra doses unless instructed by a licensed clinician.
Always use Ozempic® exactly as prescribed and keep regular follow-ups so your clinician can monitor response, side effects, and adjust dosing if needed.
Like many prescription medications, Ozempic® can cause side effects. The most commonly reported include nausea, vomiting, diarrhea, abdominal pain, and constipation—especially when starting treatment or increasing the dose. Your clinician may recommend a gradual dose escalation to improve tolerability.
Contact a clinician promptly if side effects are severe, persistent, or unusual.
Ozempic® is a prescription medicine that contains semaglutide. It belongs to a class of medications called GLP-1 receptor agonists. Ozempic® is used along with diet and exercise to improve blood sugar (glucose) in adults with type 2 diabetes, and to reduce the risk of major cardiovascular events (such as heart attack or stroke) in adults with type 2 diabetes and known heart disease.
Ozempic® is taken once weekly by injection under the skin (subcutaneous injection). Your clinician will determine whether it’s appropriate for you and how to dose it based on your medical history and goals of care.
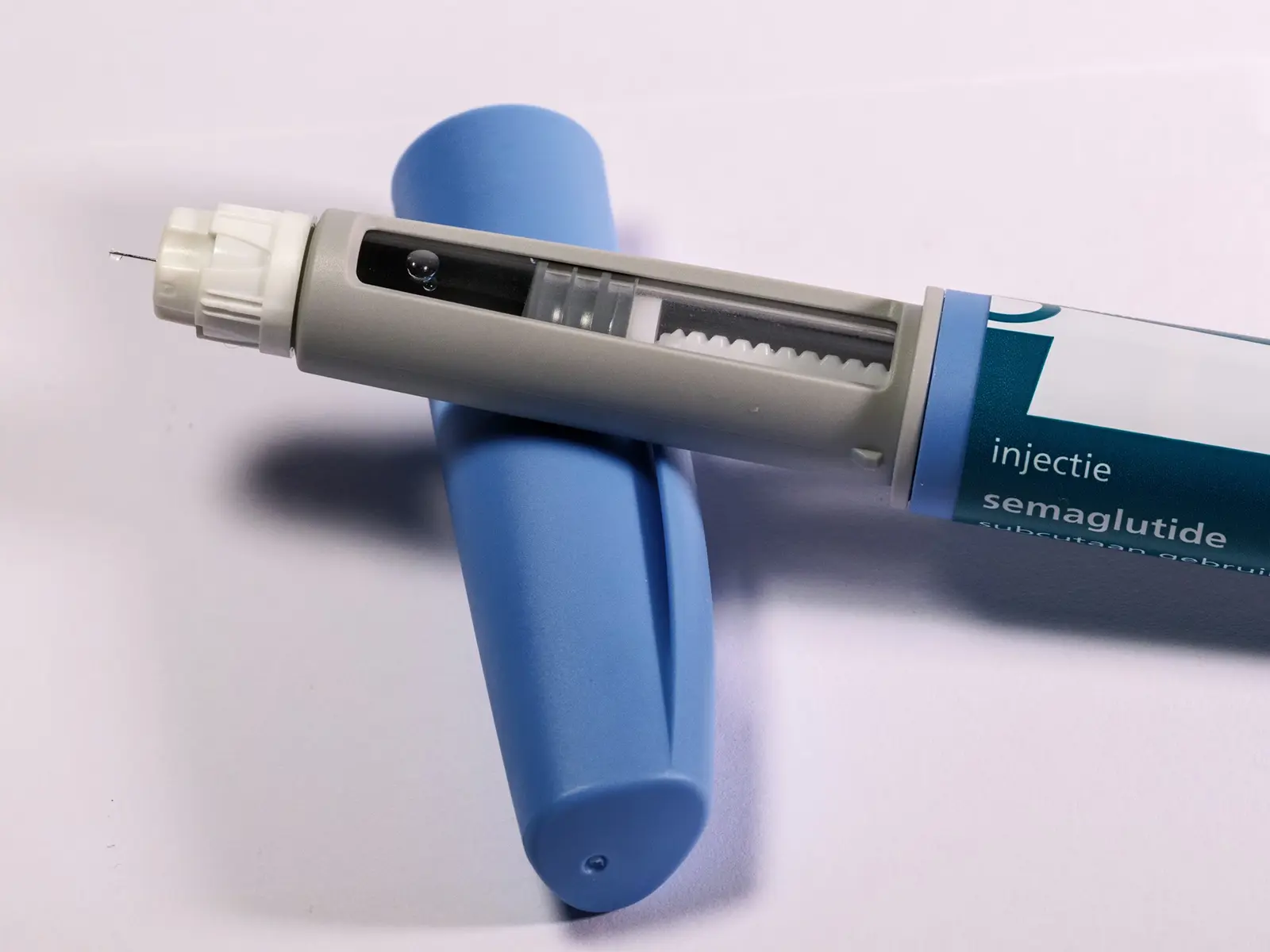
Images are for illustrative purposes only. Individual results may vary. Compounded medications are not FDA-approved.
Ozempic® works by activating GLP-1 receptors, which helps the body regulate blood sugar in several ways:
Together, these effects can help improve A1C and support healthier glucose control when used consistently and paired with nutrition and lifestyle changes.

Images are for illustrative purposes only. Individual results may vary. Compounded medications are not FDA-approved.
Ozempic® is injected once per week, on the same day each week, at any time of day, with or without food. It’s given as a subcutaneous injection (under the skin), not into a vein or muscle.
Common injection areas include:
For comfort and skin health, rotate injection sites and follow the instructions provided with your medication.

Images are for illustrative purposes only. Individual results may vary. Compounded medications are not FDA-approved.
Clinical studies of GLP-1 medications have shown weight reduction in some patients when used under medical supervision. Individual results vary.
* For illustrative estimate only.
** Estimates reflect ranges reported in clinical studies of GLP-1 medications. Individual results vary. Treatment, dosing, and outcomes are determined by a licensed clinician following clinical evaluation. Compounded medications are not FDA-approved.


Ozempic® is a brand-name prescription injection containing semaglutide. It’s FDA‑approved to improve blood sugar control in adults with type 2 diabetes and to reduce the risk of major cardiovascular events in certain adults with type 2 diabetes and heart disease. Some people also experience weight loss while taking it, but Ozempic is not specifically FDA‑approved for chronic weight management.
Weight loss can occur with semaglutide, and some clinicians may prescribe Ozempic off‑label for weight management when appropriate. Whether it’s a fit depends on your health history, goals, and medication availability—your clinician will discuss on‑label vs off‑label options and alternatives that are specifically approved for weight loss.
Semaglutide is a GLP‑1 receptor agonist. It works by mimicking a natural gut hormone that helps regulate appetite, slows stomach emptying, and improves blood sugar control—together, these effects can support reduced calorie intake over time.
A licensed clinician determines if Ozempic is appropriate based on your medical history, current medications, and clinical goals. It’s generally used for adults with type 2 diabetes; it may not be appropriate for people with certain thyroid conditions, a history of pancreatitis, or those who are pregnant or planning pregnancy.
Many people notice appetite changes within the first few weeks. Changes in weight typically build gradually over the first 8–12 weeks and continue as the dose is adjusted for tolerability and results.
The most common side effects are gastrointestinal—nausea, constipation, diarrhea, stomach discomfort, and reduced appetite—especially during dose increases. Your clinician can suggest strategies (slower titration, hydration, smaller meals) to improve tolerability. Seek medical care for severe or persistent symptoms.
Tell your clinician about your full medical history and medications, including diabetes meds, insulin, or sulfonylureas; any history of pancreatitis, gallbladder disease, kidney problems, thyroid nodules/cancer, or GI disorders; and whether you’re pregnant, breastfeeding, or trying to conceive.
Typically, you’ll complete an online intake, then have a clinician review your history and goals. If appropriate, the clinician prescribes the medication and provides a dosing plan and guidance. If prescribed through our program, medication may be delivered from a licensed pharmacy, depending on your state and plan.
Ozempic is taken as a once‑weekly injection under the skin (subcutaneous). Your clinician will provide step‑by‑step instructions on where to inject, how to store the pen, and how to rotate injection sites.
If you miss a dose, follow the instructions provided by your clinician and the medication guide. In general, the best approach is to take it as soon as you remember if it’s close to your usual schedule, or skip and resume your regular dosing day—avoid doubling doses.
Ozempic can interact with certain medications, especially other diabetes drugs that can lower blood sugar (like insulin or sulfonylureas). Always share your full medication list so your clinician can adjust doses and monitor for low blood sugar and other interactions.
Insurance coverage varies widely by plan and the medical indication. Many plans require prior authorization. We can help you understand your benefits and discuss cash‑pay options if coverage isn’t available.